 /Tan Tock Seng Hospital
/Tan Tock Seng Hospital
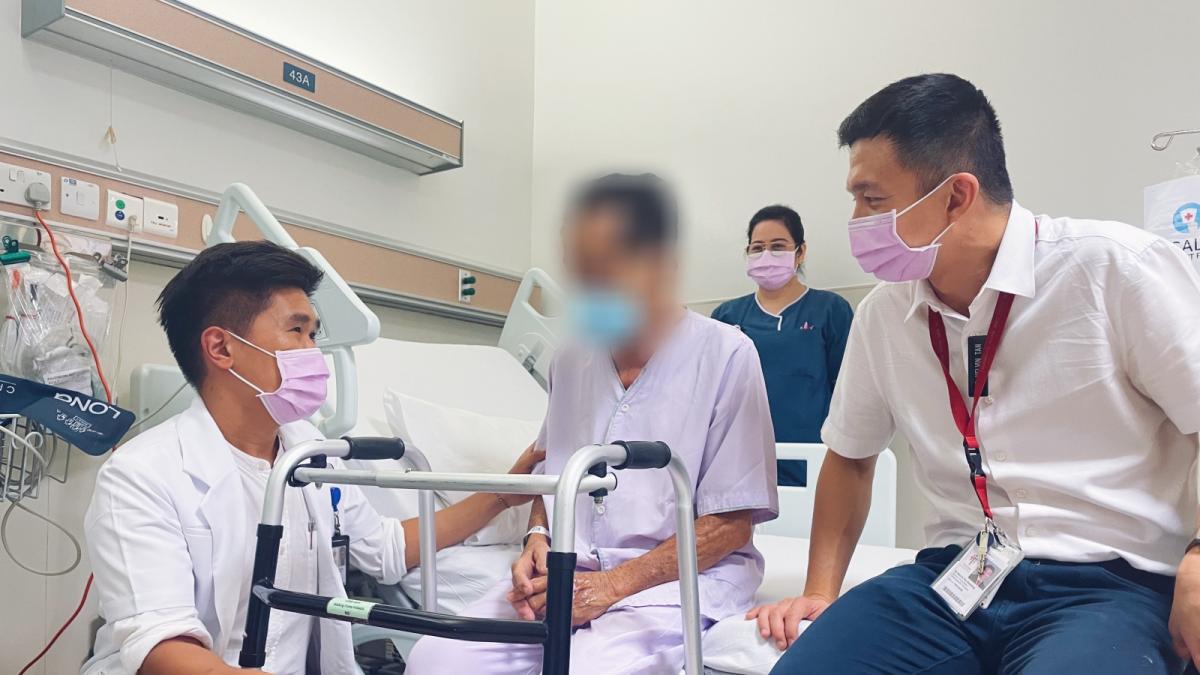
Tan Tock Seng Hospital develops remedy for overwhelmed hospitals
Its surgical care program via ambulatory setting cuts hospital stays from six to one day.
Tan Tock Seng Hospital (TTSH) performs approximately 700 knee replacement surgeries annually for older Singaporean residents with debilitating knee osteoarthritis. As a public hospital, it cannot afford to take a step back on these elective surgeries, even when COVID-19 overwhelmed its bed capacity.
What helped the hospital overcome this challenge was the enhanced recovery after surgery (ERAS) model it developed in 2017. Through ERAS, there was a progressively significant reduction in patients’ length of hospital stay, and eventually TTSH was able to perform knee replacement surgeries at its ambulatory surgery centre. Patients who undergo knee replacements are allowed to continue their healing period at home after just one to two days, some were even going home on the same day after surgery, effectively considered an outpatient procedure.
Tan Tock Seng Hospital develops remedy for overwhelmed hospitals from Charlton Media Group on Vimeo.
Partial knee replacements, a minimally invasive type of knee replacement, had previously undergone a successful trial at the TTSH Ambulatory Centre during pre-pandemic times. Building on this success, Total Knee Replacements (TKR) were integrated seamlessly into the ambulatory centre starting in January 2021, which was at the height of the COVID-19 pandemic in Singapore. This allowed TTSH to care for non-COVID patients with debilitating knee osteoarthritis whilst allowing its main hospital to continue care and treatment for COVID-19 patients.
“With our successful transition of TKR to ambulatory surgery, we could continue most of our TKR procedures in spite of manpower or bed shortage in the main building setting,” Dr. Kelvin Tan, TTSH head of adult reconstruction service, told Healthcare Asia.
TTSH plans to expand the amount of space devoted for ambulatory and day surgery by 2030 in a precinct-wide development.
ERAS shortens hospital stay and reduces costs
ERAS was introduced in 2016 for colorectal surgery and pancreas and liver surgery, amongst others. The programme was later adopted in TKR, where there are three main phases: pre-operatively, peri-operatively, and post-operatively.
Pre-operative phase involves empowering patients and changing the patient's mindset through pre-op education and optimisation of medical conditions, nutrition, and muscle strength.
Ashton Neoh, TTSH Principal Physiotherapist, said that patients started performing exercises earlier to facilitate early discharge for TKR surgery patients.
“We prepare the patient earlier at the pre-op phase. We have identified patients who are weaker or patients who have mobility levels that are not as good as the others. During the pre-op phase, the therapist or the coordinator will teach the patient some exercises so they can strengthen their legs even before they get admitted for the surgery,” said Neoh.
“It will encourage early mobilisation. Patients can start moving out from the bed and start walking around on the same day of surgery. That would facilitate their early discharge, which is not easy for the physiotherapists because it requires such a big mindset shift to do so,” he added.
In the perioperative phase, spinal anaesthesia is usually administered to allow knee replacement surgery to be performed. Medications are also given pre-emptively to reduce blood loss and therefore blood transfusions, nausea, vomiting, and giddiness episodes are avoided. This allows patients to be in the optimal state to be mobilised early post-operatively.
READ MORE: TTSH, ASUS build new AI tool for quick diagnosis of blood disorders
Lastly, the post-operative phase includes the optimisation of pain control, early mobilisation without cumbersome intravenous drips and drains, post-discharge care coordination and check back on patients.
For patients, this means an absolute reduction in costs with the ability to recover in the comfort of their own homes. For public hospitals, this allows higher turnover for elective operations, reduces bed crunch and allows the hospital to focus its resources on other emergency conditions including COVID-19 patients.
“Public [hospital] patients will tend to save more on their hospital stays as compared to patients in private hospitals, who generally wouldn’t mind paying more for an extended stay,” said Tan.
Upskilling nurses in ambulatory centre
For smoother operations at the ambulatory centre, TTSH upskills the nurses to learn the ERAS model. Neoh said they trained all surgery ward nurses to ensure that patients have enough mobility practice for early release from the hospital.
“We upskill our nurses for them to be able to help patients ambulate using different types of walking aids. We train them how to handle the patients safely and ambulate patients using different types of walking aids,” said Neoh, who is involved in the planning of ERAS protocol training for nurses.
TTSH is also eyeing to fully equip at least 60-day surgery nurses on treating knee and hip replacement surgery patients.
“It does give a sense of fulfilment for the nurses in their job as they are equipped with more knowledge and skills to handle such cases,” Adeline Tang, nurse manager of the TTSH day-surgery ward, reacting to training.
TTSH’s ERAS TKR team comprises staff from orthopaedic surgery, anaesthesia, nursing speciality, physiotherapy and occupational therapy departments involved in patients’ entire recovery journey. They provide a comprehensive and all-rounded care team for patients undergoing surgeries with the ERAS protocol.























 Advertise
Advertise










